Living with Diabetes in Prestwich? Watch for These Foot Changes
Introduction
Living with diabetes requires vigilance and awareness, particularly when it comes to foot health. At Prime Foot Clinic in Ramsbottom, Prestwich, we understand the unique challenges faced by individuals managing diabetes. Foot complications are common among diabetic patients due to nerve damage (neuropathy) and impaired circulation, which can lead to serious conditions if left unnoticed. This article will guide you through the critical foot changes to watch for and provide practical advice for maintaining optimal foot health.
What Causes Foot Changes in Diabetic Patients?
Diabetes can lead to several changes in foot health, primarily due to two factors: diabetic neuropathy and peripheral vascular disease (PVD).
- Diabetic Neuropathy: This is a type of nerve damage that can cause loss of feeling in the feet. Patients may not notice injuries, blisters, or sores, elevating the risk of infections.
- PVD: Poor blood circulation can result in slow healing and a higher risk of foot ulcers. Reduced blood flow affects the skin, making it more susceptible to cuts and abrasions that can become infected more easily.
What Common Foot Changes Should You Look For?
Individuals with diabetes should regularly inspect their feet for the following changes:
- Dry Skin: Diabetic patients may experience dry or cracked skin, particularly on the heels, which can lead to infections.
- Foot Ulcers: Open sores that do not heal are a concerning sign. Early intervention is essential to prevent worsening conditions.
- Calluses and Corns: Increased pressure on specific areas due to foot deformities (such as bunions or hammertoes) can cause the skin to harden, leading to calluses and corns.
- Changes in Skin Color: Pale or bluish skin may indicate poor circulation, warranting immediate attention.
- Fungal Infections: Athlete’s foot and toenail fungus are more common in diabetic individuals, necessitating proper foot hygiene.
How Can I Prevent Foot Problems Associated with Diabetes?
Proactive management is critical in preventing foot complications from diabetes. Consider the following preventive measures:
- Regular Foot Checks: Perform daily inspections of your feet for any abnormalities, such as cuts, blisters, or signs of infection.
- Proper Footwear: Invest in well-fitted shoes that provide adequate support and protect your feet from injuries. Avoid walking barefoot.
- Maintain Blood Sugar Levels: Keeping blood sugar levels within the target range can help prevent nerve damage and circulatory issues.
- Moisturize Your Feet: Use a good moisturizer to keep your skin hydrated, but avoid applying it between the toes to prevent fungal infections.
- Professional Foot Care: Regular check-ups with a podiatrist are essential for tailored advice and treatment options.
How Can I Treat Foot Conditions Related to Diabetes?
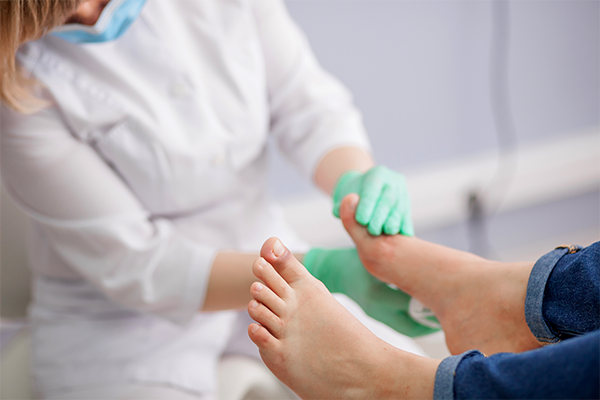
Should you notice any of the aforementioned changes, it is important to consult a podiatrist for appropriate assessment and treatment. Here are a few treatment options commonly offered:
- Diabetic Footwear: Prescription footwear can reduce the risk of ulcers and enhance comfort.
- Debridement of Wounds: A podiatrist can help clean and remove dead tissue from ulcers to promote healing.
- Topical Treatments: For infections, antifungal or antibacterial medications may be prescribed.
- Orthotics: Custom orthotics can relieve pressure on specific areas of the foot, preventing calluses and improving overall foot function.
- Regular Monitoring: Ongoing foot assessments can catch potential issues early, providing better outcomes.
When Should I See a Podiatrist?
If you experience any of the following symptoms, make an appointment with a podiatrist immediately:
- Unhealing wounds or sores
- Severe pain or swelling
- Signs of infection such as redness, warmth, or discharge
- Changes in skin color or temperature
- Numbness or tingling sensation
Frequently Asked Questions (FAQ)
1. How often should I check my feet if I have diabetes?
It is advisable to inspect your feet daily for any cuts, blisters, or changes in skin color.
2. Can diabetes cause foot deformities?
Yes, diabetes can lead to foot deformities due to nerve damage and misalignment of foot bones.
3. Are there specific exercises to help foot health in diabetics?
Exercises to improve circulation, strength, and flexibility can be beneficial. Consult with a healthcare provider for tailored recommendations.
4. What should I do if I notice a foot ulcer?
Seek immediate medical advice from a podiatrist to prevent complications and receive appropriate treatment.
5. Is it necessary to see a podiatrist regularly if I have diabetes?
Regular visits to a podiatrist are crucial for early detection and prevention of foot complications related to diabetes.
Conclusion
As a patient living with diabetes, it is vital to stay informed about potential foot changes and proactively manage your foot health. At Prime Foot Clinic in Ramsbottom, Prestwich, our expert team is here to help you navigate the complexities of diabetes-related foot issues. Don’t wait for symptoms to arise — book your appointment today for a thorough evaluation and personalized care. Schedule your visit now!